Cancer-associated thrombosis
Be clot conscious
Download the white paper on cancer-associated thrombosis
Download the patient brochure on cancer-associated thrombosis (English)
Download the patient brochure on cancer-associated thrombosis (French)
Download the patient brochure on cancer-associated thrombosis (German)
Download the patient brochure on cancer-associated thrombosis (Greek)
Download the patient brochure on cancer-associated thrombosis (Italian)
Download the patient brochure on cancer-associated thrombosis (Portuguese)
Download the patient brochure on cancer-associated thrombosis (Spanish)
Cancer is a disease with many aspects to be considered. These relate to treatment, the disease itself and the implications on your daily lifestyle. One of the most important aspects is the possibility of developing a blood clot. This condition is known as cancer-associated thrombosis (CAT).
Here are three things you need to know about cancer-associated thrombosis:
- Cancer can cause potentially fatal blood clots
- In many cases, cancer-associated thrombosis is preventable
- Cancer-associated thrombosis is treatable – provided it is caught
What is a blood clot?
Understanding deep vein thrombosis and pulmonary embolism.
Clots form when blood cells stick together, blocking blood vessels.
Deep vein thrombosis (DVT) is a clot that forms within a deep vein, usually in the leg. If untreated, part of the clot can break off and travel to the lungs, blocking blood flow. This is called a pulmonary embolism (PE), and can be potentially fatal if not detected and treated early.
Cancer and clots
The risk is real.
People with cancer have a higher than normal risk of developing a venous clot1. Indeed, blood clots are the second most common cause of preventable death in cancer patients, after infection2. Yet this condition remains under-reported, seldom discussed and often misdiagnosed3.
While all people with cancer are at some risk of developing CAT, certain people are at higher risk than others. Your risk profile will depend on:
- Type of cancer. Certain cancers have higher risk of CAT, including cancers of the stomach, pancreas, brain, kidney and ovaries, as well as hematological malignancies4.
- Stage of cancer. Cancer that is at an advanced stage can increase the risk of a clot, even in people with cancers that are otherwise considered low-risk4,5.
- Cancer treatment. Even though chemotherapy, radiation and other procedures such as surgery are vital to fight the cancer, these treatments can also cause clots6.
- Hospitalisation/immobilisation. Being confined to a bed for extended periods of time or otherwise inactive can lead to clots, in people with all types of cancer7.
- History of clots. If you’ve previously had a clot, you are three times more likely to develop CAT than people who have never had a clot8.
If you have one or more of these risk factors, you should speak to your doctor about your increased risk of CAT. Thrombosis is now considered a chronic disease in cancer patients because the risk of recurrence continues for many years after its initial incidence. You need to be vigilant.
What to look for
Recognise symptoms early. Take action fast.
CAT is not usually a silent stalker. Blood clots typically make themselves known, and can often be stopped before they become life-threatening. But you must know – and be alert to – the signs and symptoms.
Speak to your doctor or nurse immediately if you experience any of the following symptoms of deep vein thrombosis:
- Swelling in the foot, ankle, leg or arm (skin may feel stretched), particularly if it appears on only one side
- Pain, cramping or tenderness, often in the calf
- Redness or noticeable discoloration of the leg or arm
- Warm or heavy sensation in the leg
Contact emergency services immediately if you experience any of the following symptoms of pulmonary embolism:
- Light-headedness/dizziness
- Unexplained shortness of breath
- Irregular heartbeat
- Chest pain (especially when breathing deeply)
- Coughing up blood
Always err on the side of caution…
Some people may mistake CAT symptoms for normal side effects of cancer treatment. However, if you are in any doubt at all, seek medical attention straight away.
Treating CAT
Dealing with CAT and preventing recurrence.
Treatment for CAT is effective and relatively simple.
DVT and PE are most often treated with anticoagulants (often referred to as “blood thinners”, though they don’t actually thin the blood, but rather slow the clotting process).
Anticoagulants prevent new clots from developing and stop existing clots from growing. Treatment should continue for at least six months to prevent recurrence.
One of the main side effects of anticoagulant therapy is the risk of bleeding. In most cases, this should not deter you from seeking treatment.
Treatment prevents clots from getting larger and lowers the chance of new clots forming9.
Prevention
Minor lifestyle changes can make a difference.
Four easy steps to reduce your risk of CAT:
- Keep moving: stretch your legs, move your feet, take a little walk
- Quit smoking: support is there if you want it
- Stay hydrated: drink plenty of fluids, avoid alcohol and caffeine
- Wear prescribed compression socks/stockings
Have a conversation
Three questions to ask your doctor:
- What is my risk for CAT?
- What should I look out for?
- If I’m concerned I have CAT, what should I do?
Cancer-associated thrombosis (CAT) survey
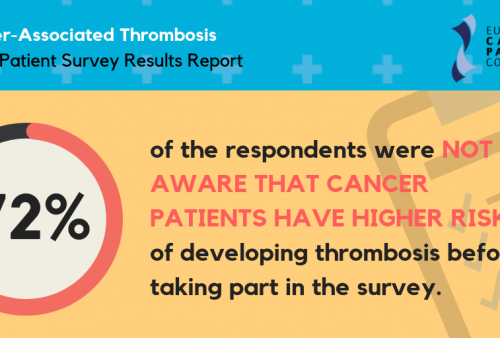
The European Cancer Patient Coalition ran a survey to get a better picture of the awareness on Cancer-Associated Thrombosis among people with cancer in Europe. The survey, which was carried out in 2018 in several European countries, revealed very low awareness about cancer associated thrombosis among cancer patients in Europe. A vast majority of respondents said that, before taking part in the survey, they were unaware that people with cancer have a higher than normal risk of developing thrombosis. The remaining 28% of patients responded that they were previously aware of it.
Despite the remaining 28% respondents’ awareness of the increased risk of thrombosis for cancer patients, the level of understanding was reported to be low.
More needs to be done by clinicians and patient organisations, at every stage of the cancer journey, to ensure that the risks of cancer-associated thrombosis are better known. Health professionals should provide more information for patients at the time of the cancer diagnosis, and also at follow-up appointments.
As well as providing information about cancer-associated thrombosis verbally, doctors and nurses need to provide written information or provide information about credible resources on-line to cancer patients that they can access and refer to. Given that cancer patients often need, or choose, to seek information about cancer-associated thrombosis on-line, healthcare providers and patient organisations need to do more to ensure that such information is available, clear and consistent.
Click here to download the Cancer-Associated Thrombosis Survey Report.
Click here to download the Executive Summary of the Cancer-Associated Thrombosis Survey Report.
Own your health.
Be clot conscious.
Speak to your healthcare professional today.
References:
1. Chew H, et al. Incidence of Venous Thrombembolism and its effect on survival among patients with common cancers. Arch Intern Med. 2006;166:458. 2. Trujillo-Santos J, Martos FM, Font C, Farge-Bancel D, Rosa V, Lorenzo A, Barrón M, Lorente MA, Pedrajas JM, Monreal M. Heliyon. 2017 Jan 16;3(1):e00229. doi: 10.1016/j.heliyon.2016.e00229. eCollection 2017 Jan. 3. Noble S, et al. Patients’ Experiences of LIving with CANcer-associated thrombosis: the PELICAN study. Patient Prefer Adherence. 2015;9:337-45. 4. Young AM, Chapman O, Connor C, Poole C, Rose P, Kakkar AK. (2012); Thrombosis and Cancer. Nat Rev Clin Oncol. 9(8):437-49. 5. Lyman GH. (2011) Venous thromboembolism in the patient with cancer. Cancer. [online]. 117:1334–1349. 6. Hiller E. Cancer and thrombosis: managing the risks and approaches to thromboprophylaxis – Review sheet. 7. Thrombosis Canada. Cancer-Associated Thrombosis (CAT) – Patient Information Sheet. http://thrombosiscanada.ca/wp-content/uploads/2016/10/M159-Cancer-Associated-Thrombosis_Oct2016.pdf. 8. National Blood Clot Alliance. Cancer and Blood Clots – Fast Facts https://www.stoptheclot.org/cancer-and-blood-clots-fast-facts.htm (accessed 29-May-2017). 9. National Blood Clot Alliance. Blood Clot Treatment. https://www.stoptheclot.org/learn_more/blood_clot_treatment (accessed 29-May-2017).
Names and affiliations of experts that helped develop this material:
Prof. Jacob C. Easaw, Associate Professor in the Division of Medical Oncology at The Tom Baker Cancer Center, Calgary, Alberta; Prof. Ismaïl Elalamy, Professor of Haematology and Head of the Haematology Department at Tenon University Hospital, Paris, and current President of the French Society of Angiology; Evelyn Knight, Co-Founder and Chief Executive, AntiCoagulation Europe; Sofia Leonardou, member of B.D. K.E.F.I association; Dr. Lydia E Makaroff, European Cancer Patient Coalition; Prof. Manuel Monreal, Clinical Professor of Internal Medicine at the Faculty of Medicine, Universidad Autónoma in Barcelona and Head of Internal Medicine at the Hospital Universitari Germans Trias i Pujol in Barcelona, Spain; Dr. Ana Rosa Rubio, Board Certified Oncology Pharmacist, Complejo Hospitalairo de Toledo, Spain; Prof. Annie Young, Professor of Nursing at the University of Warwick, UK.
LEO Pharma A/S has provided support to the development of the patient information via the engagement of the independent agency Copentown, who has facilitated the development of the brochure with the ECPC and the expert group.